Here’s a snapshot of the different Medicare watchdogs and some of the other government agencies that oversee health care organizations. It was developed by Frank Mesaros, manager of compliance risk & facility audits at WellSpan Health in York, Pennsylvania, to help employees get a better sense of the differences among them. “We found it helpful when looking at an issue and thinking about all the possible implications and who might be responsible for oversight,” added Wendy Trout, director of corporate compliance at WellSpan. Contact Mesaros at fmesaros@wellspan.org and Trout at wtrout@wellspan.org.
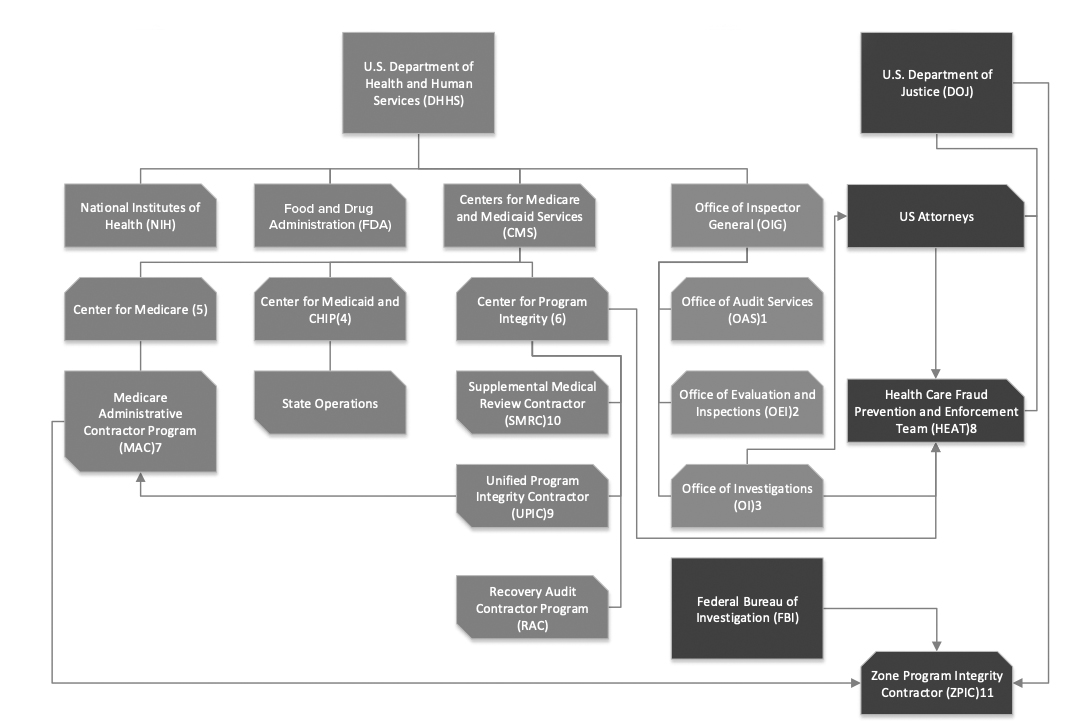
NOTE: This chart is not intended to be all inclusive, was based on our current understanding at the time, and is not an official government document. Created by Frank Mesaros, Manager, Compliance Risk & Facility Audits, WellSpan Health.
Integration Chart Notes
-
OAS: The Office of Audit Services conducts independent audits of HHS programs and/or HHS grantees and contractors. These audits examine the performance of HHS programs and/or grantees in carrying out their responsibilities and provide independent assessments of HHS programs and operations.
-
OEI: The Office of Evaluation and Inspections conducts national evaluations of HHS programs from a broad, issue-based perspective. The evaluations incorporate practical recommendations and focus on preventing fraud, waste or abuse and encourage efficiency and effectiveness in HHS programs.
-
OI: The Office of Investigations conducts criminal, civil and administrative investigations of fraud and misconduct related to HHS programs, operations and beneficiaries. State-of-the-art tools and technology assist Office of Inspector General (OIG) investigators around the country and help OI meet its goal of becoming the world’s premier health care law enforcement agency.
-
Center for Medicaid and CHIP:
-
Serves as CMS’s focal point for assistance with formulation, coordination, integration and implementation of all national program policies and operations relating to Medicaid, the Children’s Health Insurance Program (CHIP), and the Basic Health Program (BHP).
-
In partnership with states, assists state agencies in successfully carrying out their responsibilities for effective program administration and beneficiary protection, and, as necessary, supports states in correcting problems and improving the quality of their operations.
-
Identifies and proposes modifications to Medicaid, CHIP and BHP program measures, regulations, laws, and policies to reflect changes or trends in the health care industry, program objectives, and the needs of Medicaid, CHIP, and BHP beneficiaries. Collaborates with the Office of Legislation on the development and advancement of new legislative initiatives and improvements.
-
Serves as CMS’s lead for management, oversight, budget and performance issues relating to Medicaid, CHIP, BHP and the related interactions with states and the stakeholder community.
-
Coordinates with the Center for Program Integrity on the identification of program vulnerabilities and implementation of strategies to eliminate fraud, waste and abuse. Leads and supports all CMS interactions and collaboration relating to Medicaid, CHIP and BHP with states and local governments, territories, Indian Tribes and tribal healthcare providers, key stakeholders (e.g., consumer and policy organizations and the health care provider community) and other federal government entities. Facilitates communication and disseminates policy and operational guidance and materials to all stakeholders, and works to understand and consider their perspectives, support their efforts and develop best practices for beneficiaries across the country and throughout the health care system.
-
-
Center for Medicare:
-
Serves as CMS’s focal point for the formulation, coordination, integration, implementation and evaluation of national Medicare program policies and operations.
-
Identifies and proposes modifications to Medicare programs and policies to reflect changes or trends in the health care industry, program objectives and the needs of Medicare beneficiaries. Coordinates with the Office of Legislation on the development and advancement of new legislative initiatives and improvements.
-
Serves as CMS’s lead for management, oversight, budget and performance issues relating to Medicare Advantage and prescription drug plans, Medicare fee-for-service providers and contractors.
-
Oversees all CMS interactions and collaboration with key stakeholders relating to Medicare (e.g., plans, providers, other government entities, advocacy groups, Consortia) and communication and dissemination of policies, guidance and materials to understand their perspectives and to drive best practices in the health care industry.
-
Coordinates with the Center for Program Integrity on the identification of program vulnerabilities and implementation of strategies to eliminate fraud, waste and abuse.
-
-
Center for Program Integrity:
-
Serves as CMS’s focal point for all national and statewide Medicare and Medicaid programs and CHIP integrity fraud and abuse issues.
-
Promotes the integrity of the Medicare and Medicaid programs and CHIP through provider/contractor audits and policy reviews, identification and monitoring of program vulnerabilities, and providing support and assistance to states. Recommends modifications to programs and operations as necessary and works with CMS centers, offices and the chief operating officer (COO) to effect changes as appropriate. Collaborates with the Office of Legislation on the development and advancement of new legislative initiatives and improvements to deter, reduce, and eliminate fraud, waste, and abuse.
-
Oversees all CMS interactions and collaboration with key stakeholders relating to program integrity (e.g., U.S. Department of Justice, HHS OIG, state law enforcement agencies, other federal entities, CMS components) for the purposes of detecting, deterring, monitoring, and combating fraud and abuse, as well as taking action against those that commit or participate in fraudulent or other unlawful activities.
-
In collaboration with other CMS centers, offices and the COO, develops and implements a comprehensive strategic plan, objectives and measures to carry out CMS’s Medicare, Medicaid and CHIP program integrity mission and goals, and ensure program vulnerabilities are identified and resolved.
-
-
A/B MACs: A/B Medicare administrative contractors process Medicare Part A and Medicare Part B claims for a defined geographic area or “jurisdiction,” servicing institutional providers, physicians, practitioners and suppliers.
-
Home Health and Hospice MACs: There are four A/B MACs that process home health and hospice claims in addition to their typical Medicare Part A and Part B claims. Please note that the four home health and hospice areas do not coincide with the jurisdictional areas covered by these four A/B MACs.
-
DME MACs: The durable medical equipment MACs process Medicare durable medical equipment, orthotics, and prosthetics (DMEPOS) claims for a defined geographic area or “jurisdiction,” servicing suppliers of DMEPOS.
-
-
HEAT: Since June 2011, CMS uses the Fraud Prevention System (FPS) on all Medicare fee-for-service claims on a streaming, national basis. Similar to the fraud-detection technology used by credit card companies, FPS applies predictive analytics to claims before making payments in order to identify aberrant and suspicious billing patterns. CMS uses leads generated by FPS to trigger actions that can be implemented swiftly. Early results from FPS show significant promise. Since 2011, the FPS identified savings (certified by HHS OIG) associated with these prevention and detection actions were $820 million. This resulted in more than a 10-to-1 return on investment for the first three years of implementation.
-
UPIC: Unified program integrity contractors’ primary goal is to investigate instances of suspected fraud, waste, and abuse in Medicare or Medicaid claims. They identify any improper payments that are to be recouped by the MAC.
-
SMRC: With CMS-directed topic selections and time frames, the supplemental medical review contractor conducts nationwide medical reviews (Part A, Part B and DME) in accordance with all applicable statutes, laws, regulations, national and local coverage determination policies, and coding guidance to determine whether Medicare claims have been billed in compliance with coverage, coding, payment and billing practices. Such reviews are assigned through CMS formal notifications and focus on analysis of national claims data issues identified by federal agencies, such as the OIG, Government Accountability Office (GAO), CMS internal data analysis, the Comprehensive Error Rate Testing (CERT) program, and professional organizations, and/or analysis reports such as First-Look Analysis Tool for Hospital Outlier Monitoring (FATHOM) report and Program for Evaluating Payment Patterns Electronic Report (PEPPER). Reviews are based upon Provider Compliance Group (PCG), Program Integrity (PI), Healthcare Fraud Prevention Partnership (HFPP) project types.
-
ZPIC: Once a fraud or abuse issue is identified within a MAC jurisdiction, it is escalated to a zone program integrity contractor. ZPICs work with the Department of Justice and the FBI when the likelihood of fraud is high. ZPICs have the power to suspend claims for up to a year without any appeal rights.
